Helena O. Taylor MD, PHD, FACS & Stephen R. Sullivan MD, MPH, FACS
Named Among the Best Plastic Surgeons in Boston
We enjoy collaborating with our general surgery colleagues in the treatment of complicated abdominal wall defects and hernias. When a patient has had multiple prior surgeries, multiple scars, or other complicating factors we often perform surgery as a team, to minimize risk and maximize benefit.
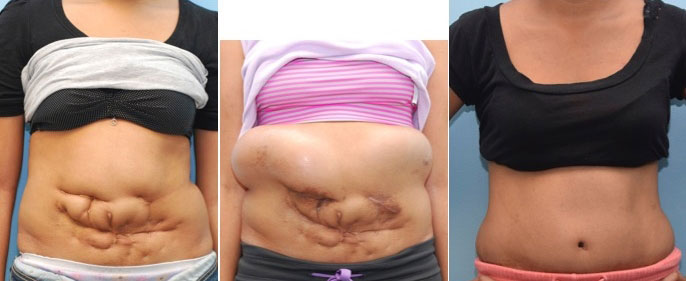
This young woman had a particularly complicated form of abdominoplasty (tummy tuck) and abdominal wall reconstruction due to a past history of multiple abdominal operations as a child. Preoperatively (left), she had extensive scaring, many hernias and no obvious umbilicus (belly button). Activities that many of us take for granted, such as swimming, summer time in a bathing suit, or form fitting clothing, were a source of fear or embarrassment.
Dr. Taylor and Dr. Sullivan made a plan for tummy tuck and complex abdominal reconstruction and placed tissue expanders (center), which they slowly inflated to stretch the skin. Several weeks later, the scarred skin was then removed, the hernias repaired, and the belly button reconstructed. Several months postoperatively (right) a normal appearance has been restored and her life has been changed with scars hidden below underwear lines. She can now enjoy summer months and swimming with friends with few people knowing about her operations.
WHAT ABDOMINAL RECONSTRUCTION DOES
DURATION OF RESULT
Years
LENGTH OF PROCEDURE
3-4 hours
TYPES OF ANESTHESIA
General Anesthesia
RECOVERY
TIME OFF SCHOOL OR WORK
TIME OFF ACTIVITIES
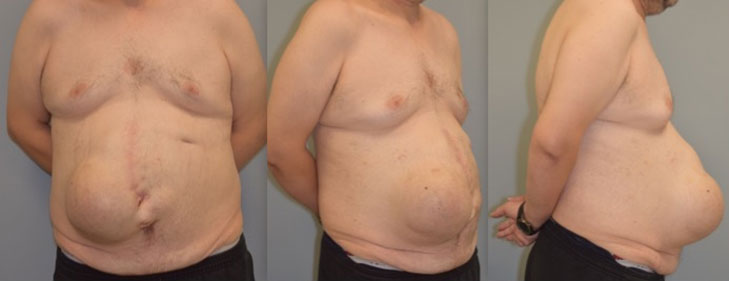
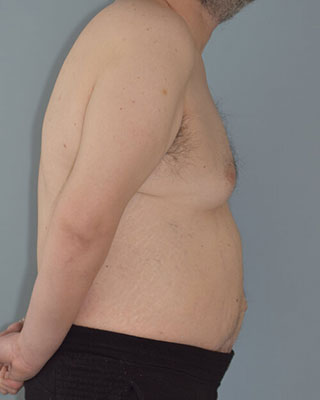
Man with history of multiple abdominal operations and attempts at hernia repair by other surgeons who is left with recurrent ventral, incision and umbilical hernias, abdominal bulge, abdominal scars. Dr. Taylor, Dr. Sullivan and Dr. Gutweiler performed abdominal reconstruction.
Diastasis recti refers to the separation of the vertical rectus muscles of the abdomen which most often happens with pregnancy, but can also occur with age and changes in weight. This widening of the space between the abdominal muscles can cause a bulge, and weakening of the core. Unlike a hernia however there is no true hole in the fascial layer, just a thinning and lateral migration. Diastasis repair plays an integral role in most tummy tuck or cosmetic abdominoplasty procedures, but may also be performed to reinforce a hernia repair. While we often feel that this muscular repositioning is a functional or reconstructive procedure, most (dare we say all) insurance carriers consider diastasis recti repair to be a cosmetic procedure.
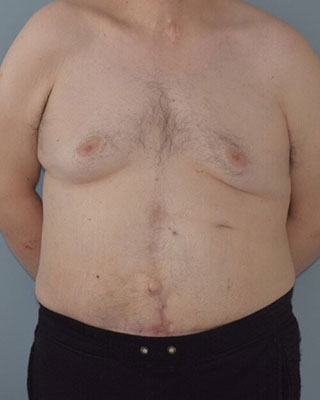
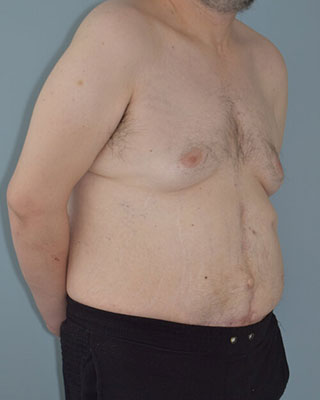
Same man shown above more than one year after after abdominal reconstruction with Dr. Taylor, Dr. Sullivan, and Dr. Gutweiler.
The hernia was repaired using a low transverse incision, the same approach used with an abdominoplasty or “tummy tuck”. The scar is hidden in the underwear line. This approach is used to improve exposure and improve safety and recovery. The hernia was repaired with mesh using the Rives-Stoppa technique, which has the lowest rate of hernia recurrence. Abdominal wall component separation is also used to repair the muscle layers. Finally, excess skin is removed.
WOUND CARE
ACTIVITY
GENERAL OUTCOMES
It is important to be seen by Dr. Taylor or Dr. Sullivan after your operation. They will see you in follow-up appointments at 1 week, 3-4 weeks, 3-6 months, and 1 year or as often as needed post-op. Call Taylor and Sullivan Plastic Surgery to schedule your appointments at (617) 492-0620 between the hours of 8:30 – 5:00 or visit our webpage at www.massplasticsurgeons.com. We are always available for postoperative concerns or emergencies and can be reached through our paging service 24 hours per day at (617) 492- 0620.
Download our Abdominoplasty (Tummy Tuck) postoperative instructions.
Call Today 617.492.0620
To schedule a private consultation with Dr. Taylor or Dr. Sullivan, please call the office or request an appointment using our form. We welcome your visit and your questions.
300 Mount Auburn St. Ste 304, Cambridge, MA 02138





